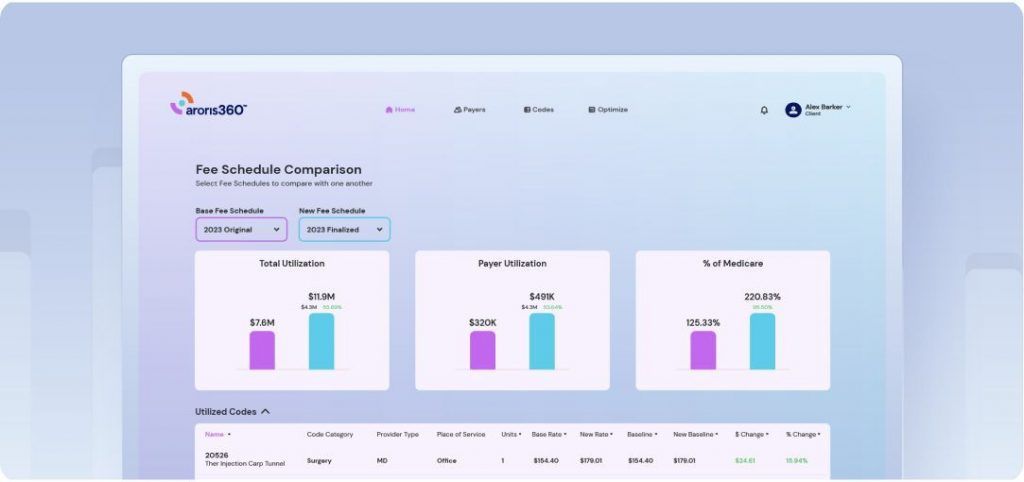
Become the next
Aroris success story.
See what a healthy dose of data can do for your practice’s well-being.
CASE STUDIES
A Midwest Behavioral Health Group
Turning a loss into a 20-point victory.
Aroris uses its insider expertise to help a behavioral healthcare provider reverse a rate decrease.
Rate increase
A Northeast Orthopedic Group

Doing what thought couldn’t be done.
Aroris earns increases on previously non-negotiable payer contracts for a provider with multiple entities.
Rate increase
A Midwest Multi-Specialty Group
Saving a relationship for a community’s good.
Aroris makes the case that reimbursement rate adjustments were needed for a provider to stay in the provider’s network.
Rate increase

A Northeast Anesthesiology Group

Transforming a shortfall into a windfall.
Aroris leverages digital technology and analytical expertise to spot reimbursement revenue opportunities.
Rate increase
Northwest Pain Management practice

Negotiating a profitable future by engaging proactively.
Aroris expertly counters drastic fee changes, securing fair reimbursements and driving significant revenue growth for healthcare practices.
Rate increase
Southwest Cardiology Practice

Appealing to the payer’s competitive needs.
Aroris transforms complexity into opportunity, ensuring fair compensation and superior patient care in healthcare.
Rate increase
Midwest Optometry and Ophthalmology Practice

Designing alternative solutions to achieve win/win results.
Aroris champions equitable healthcare, maintains fair fee schedules and enhances revenue for healthcare providers.
Rate increase

Southwestern Behavior Health Provider

Not settling for the status quo.
Aroris detangles complexity to focus on what matters most.
Rate increase
Southeastern Orthopedic Group

Correcting an unfair deal.
Aroris persistently appeals to good faith and fair dealing to earn a more equitable payer contract.
Rate increase